Diabetic Retinopathy Specialist
Damage to the blood vessels in the tissue at the back of the eye causes diabetic retinopathy (retina). A risk factor is poorly regulated blood sugar. Floaters, blurriness, dark patches of vision and difficulties detecting colors are early signs. Blindness is a possibility. Diabetes can be managed carefully with mild symptoms. Advanced instances may necessitate laser therapy or surgery. Routine eye exams and proper diabetes management can help stop diabetic retinopathy from worsening. Visit our board-certified ophthalmologists for diabetic retinopathy treatment at Connecticut Retina Consultants. Contact us for more information. We serve patients at locations in Hamden, New Haven, Madison, Trumbull, Fairfield, and Norwalk CT.
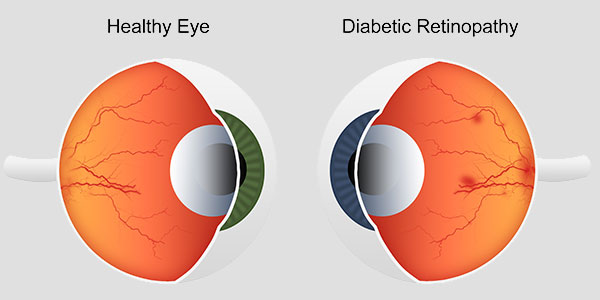
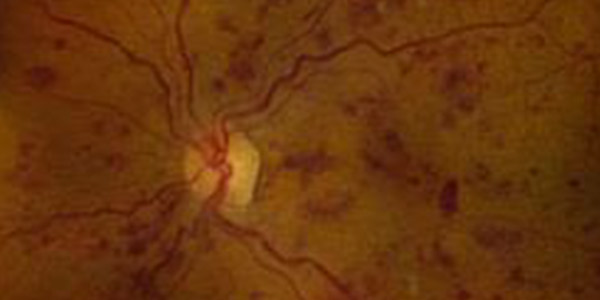
Table of Contents:
Can diabetic retinopathy be corrected?
What are the warning signs of diabetic retinopathy?
What worsens diabetic retinopathy?
How do you stop diabetic retinopathy from progressing?
Diabetes affects 16 million Americans and is the leading cause of new cases of blindness in people ages 20 to 74. Each year 12,000-24,000 people will lose their sight from the disease. Vigilant care, particularly controlling one’s blood sugar, blood pressure and cholesterol can reduce the risk of vision complications from diabetes. For those that do develop problems, various treatments offer hope for saving or recovering some sight.
What is diabetes?
Diabetes is a chronic disease in which the body does not produce or properly use insulin, a hormone that helps convert sugar and food into energy. The biochemical reactions that occur because the body doesn’t have the proper means of regulating blood sugar can have a profound impact on the eyes. A high sugar level thickens the lens and bends the light that filters through. When sugar levels decrease, just the opposite happens. The constant thickening and thinning of the lens due to dramatic swings in blood sugar levels leads to blurry vision and increases the risk of cataract formation. For people who are unaware that they have diabetes, blurry vision may be the first sign that something is amiss. For those who know they are diabetic, blurry vision may be a reflection of poorly controlled blood sugar levels. Improved control through a combination of diet, exercise and medication can be very helpful in preventing secondary complications of diabetes including vision loss.
What is diabetic retinopathy?
The chemical changes caused by diabetes can damage blood vessels throughout the body, including the fine blood vessels in the retina. This damage is called diabetic retinopathy, of which there are two kinds:
Non-proliferative diabetic retinopathy (NPDR) occurs when the retinal blood vessels start to leak, causing blood or fluid to seep into the retina. The retina becomes thick and swollen and does not work correctly. If the leaking happens in the macula, (the central part of the retina), vision will be blurred from macular edema. If the leaks occur on the periphery of the retina, there may be no immediate impact on vision.
Proliferative diabetic retinopathy (PDR) occurs when the retinal blood vessels close, cutting off nutrition to the retinal tissue. Abnormal new blood vessels, called neovascularization, may form and cause bleeding and scar tissue. The bleeding (called vitreous hemorrhage because the blood fills up the vitreous cavity inside the eye) and scar tissue can result in blindness if not treated. The earlier neovascularization is discovered, the better the chance that surgery can save vision.
Both types of diabetic retinopathy may occur without a noticeable change in vision. It is therefore imperative, if you have diabetes, to have your retinas examined at least once every 12 months, and more often than that if you have already developed significant retinopathy.
How is diabetic retinopathy treated?
For patients with NPDR and diabetic macular edema, laser surgery can seal the blood vessels to stop leaking and prevent further vision loss. Typically a circulation study (fluorescein angiogram) is performed in the office to pinpoint the exact locations of the leaks. Ocular coherence tomography (OCT) is also often performed to evaluate the extent of macular edema. Even after laser surgery is done, new leaks may develop or sealed leaks may reopen, requiring additional laser treatments. Over the last several years, several medications have been developed to effectively treat edema as well. The medications can be injected painlessly into the eye in the office to treat macular edema that does not respond to laser or that can not be safely lasered. That is why it is very important to check your vision one eye at a time routinely and report any changes or blurriness to your doctor.
Severe neovascularization resulting from PDR can also be treated with in-office laser surgery to prevent severe vision loss. For patients who don’t respond to the laser, and develop recurrent bleeding or tractional scar tissue membranes, retina surgery called “vitrectomy” may be indicated. A vitrectomy removes the jelly-like substance in the center of the eye, called the vitreous. This is where the abnormal diabetic blood vessels and hemorrhaging are located, so the vessels and blood are removed with the vitreous. Any scar tissue that has formed is also removed.

Additional Treatments You May Like

Additional Treatments You May Like
- Macular Degeneration
- Scleral Buckling
- Uveitis
- Macular Edema
- Photodynamic Therapy (PDT)
- Degenerative Myopia
- Laser Photocoagulation
- Retinal Detachment
- Diabetic Retinopathy
- Lattice Degeneration
- Pneumatic Retinopexy
- OCT
- BRVO
- Inherited Retinal Disorders
- Macular Hole
- Flashes and Floaters
- Macular Pucker
- Angiography
- CRVO
- Cryotherapy
- Retinal Artery Occlusion
- Intravenous Fluorescein Angiogram
- Retinal Tear
- Vitrectomy
- AMD
- Intravitreal Injections
- Complications After Cataract Surgery
- CSCR
- Pars Plana Vitrectomy




