Age-Related Macular Degeneration (AMD)
AMD is the leading cause of vision loss among older adults, but early detection and treatment can limit complications. A person’s central vision is affected by age-related macular degeneration (AMD). AMD can cause severe central vision loss, however, it seldom causes blindness. Being 50 or older, smoking, having high blood pressure, and eating a high-fat diet are all risk factors for AMD. The occurrence of metamorphoses, in which images are viewed in a twisted manner, is the most telling indication. In addition to an eye examination, several exact tests are required to identify maculopathy. AMD treatment is available at Connecticut Retina Consultants. Contact us for more information. We serve patients at locations in Hamden, New Haven, Madison, Trumbull, Fairfield, and Norwalk CT.


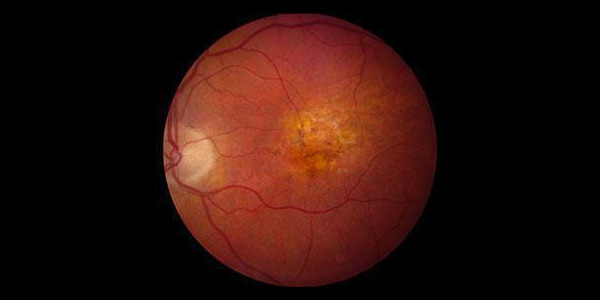
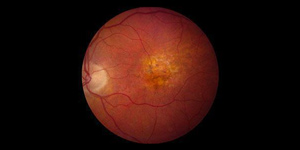
Table of Contents:
What is AMD?
What are the main causes of AMD?
How can I stop macular degeneration from getting worse?
At what age does macular degeneration usually begin?
Age-related macular degeneration (AMD) is the leading cause of blindness in people over the age of 65 in the United States. The macula is the central area of the retina that controls fine detailed vision. At least 10 million Americans have some form of macular degeneration. Over 3 million Americans currently have “advanced” AMD. It is estimated by 2050 5.5 million Americans will have the advanced form of this disease. As the disease advances, progressive blurring of the central vision can occur. Peripheral (side) vision is generally not affected even in advanced stages.
The most common form of AMD is “dry” AMD. In this condition, there is a slow deterioration of retinal cells and their supportive cells. There is a progressive atrophy (thinning) of the macula and deposition of retina cell waste products (drusen) that your doctor can see under the slit lamp microscope. While dry AMD can affect one’s vision, it is usually slowly progressive but may result in significant visual impairment. In addition to a special formulation of vitamins proven by the Age Related Eye Disease Study (AREDS) to slow the progression of the disease and reduce the chance of dry AMD converting to wet AMD by 25%, new therapies were approved in 2023 (Syfovre) to further slow progression. These medications are administered in the office to appropriate candidates. Please speak with your doctor to see if you qualify for these new treatments.
“Wet” AMD is the more potentially devastating form of the disease. 10-20%% of patients with dry age-related macular degeneration will progress over time to “wet”. It is termed “wet” because blood or fluid can leak into, or under, the center part of the macula causing distorted images (metamorphopsia) and permanent vision loss. Wet AMD occurs more rapidly, thus please call your doctor if you notice any sudden worsening of your vision or new distortion or wavy lines. Fortunately, great advances have been made in the treatment of wet AMD in the form of specialized medications called anti-VEGF agents.
These medications are administered in the office as an injection. Treatments are typically painless and very effective in halting progression of the disease. Each patient requires a particular regimen of these medications including dosage, medication type, and treatment intervals. At Connecticut Retina Consultants, we choose from all available anti-VEGF medications including Avastin® (bevacizumab), Lucentis (ranibizumab), Eylea® (aflibercept), Beovu, and Vabysmo to achieve the best efficacy. Sometimes, supplemental treatment with photodynamic therapy (PDT) or steroid injections may help.

Additional Treatments You May Like

Additional Treatments You May Like
- Macular Degeneration
- Scleral Buckling
- Uveitis
- Macular Edema
- Photodynamic Therapy (PDT)
- Degenerative Myopia
- Laser Photocoagulation
- Retinal Detachment
- Diabetic Retinopathy
- Lattice Degeneration
- Pneumatic Retinopexy
- OCT
- BRVO
- Inherited Retinal Disorders
- Macular Hole
- Flashes and Floaters
- Macular Pucker
- Angiography
- CRVO
- Cryotherapy
- Retinal Artery Occlusion
- Intravenous Fluorescein Angiogram
- Retinal Tear
- Vitrectomy
- AMD
- Intravitreal Injections
- Complications After Cataract Surgery
- CSCR
- Pars Plana Vitrectomy




